Filter Resources

Public-private data project a COVID game-changer in West and East Africa
The USAID-funded Regional Action Through Data (RAD) programme launches game-changing daily COVID dashboards in West and East Africa and a ground-breaking childhood cross-border immunisation programme that could be a model for future COVID passport initiatives across these regions
A cross-border data collaboration project involving 23 African countries above the Equator is proving to be a game-changer for the tracking and management of COVID-19 and other epidemic-prone diseases in the region – and is launching the first ever daily public COVID dashboard for countries in the Horn of Africa next month.
The USAID-funded Regional Action Through Data (RAD) programme is tackling COVID-19 in West and East Africa through two initiatives, respectively involving the sharing of real-time regional disease data online and tech-enabled cross-border immunisations. These initiatives are enabling governments to better collaborate to protect their roving pastoral populations from epidemics and to overcome the data issues of the Ebola era.
Game-changing COVID-19 dashboards enable daily regional epidemic tracking
Ebola became a deadly disaster six years ago due to inadequate and irregular, at best weekly, information sharing among affected countries. But this scenario will soon be a thing of the past, with the Intergovernmental Authority on Development (IGAD) trade bloc in Central and East Africa getting its own daily online disease outbreak dashboard before the end of June 2021. Currently the tracker shows monthly graphs, but soon new daily regional information will be available as well. The dashboard allows its eight member countries in the Horn of Africa, Nile Valley and African Great Lakes regions to share epidemic data on a daily basis for the first time.
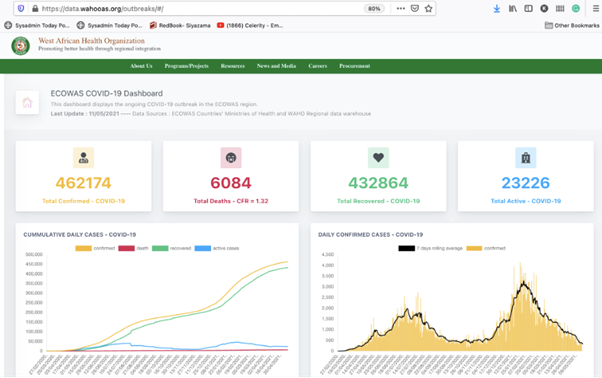
The IGAD dashboard follows on RAD’s recently unveiled “disease outbreak dashboard” for the West African Health Organization (WAHO). The WAHO COVID-19 Dashboard is freely available on the WAHO website and offers information, maps and tables to reflect how COVID is manifesting daily in the region. It will soon also track other epidemic-prone diseases. WAHO is the health arm of the Economic Community of West African States (ECOWAS) and serves 15 countries including Ghana, Nigeria and Mali.
The RAD programme was launched in 2016 in response to the Ebola pandemic to identify and co-create actionable solutions for pressing African health needs and pivoted to deal with COVID last year. It is a USAID collaboration with both WAHO and IGAD, with implementation led by BroadReach Health Development.
Implementation partner BroadReach’s health-tech experts are providing prime oversight and support, in collaboration with Duke University and Jembi Health Systems NPC, who provide policy and technical support.
These publicly accessible online dashboards are an absolute game-changer for all partnering countries, especially in jointly managing the health of migratory populations in real-time, says Geoffrey Arunga, Regional Analyst for the RAD project in BroadReach, who manages the data functionality of the dashboards.
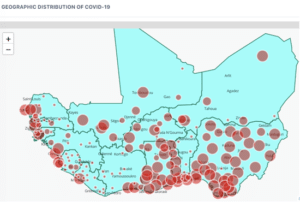
WAHO’s online COVID map reveals daily hotspots across West Africa
Dr. Andrew Kitua, BroadReach’s Regional Programme Director of RAD, who manages the implementation of the programme, says: “The emergence of COVID-19 has again highlighted how diseases can emerge from anywhere and spread rapidly across continents in this globalised era, but now through our RAD work we are able to use real-time data sharing to empower health authorities to respond immediately to outbreaks – outbreaks that have no respect for borders.”
This kind of data-sharing could future-proof Africa against the next pandemic, by driving the supply of data, sharing and policy, and managing actual demand for health products and production, said Kitua. It also motivates health workers who can now see the fruits of their labour and “helps defeat COVID denialism” in political leaders who are now confronted with robust regional data.
Ground-breaking cross-border childhood immunisation programme
IGAD which comprises Djibouti, Eritrea, Ethiopia, Kenya, Somalia, South Sudan, Sudan and Uganda, has also launched a ground-breaking cross-border childhood immunisation programme, called the “Journey Solution”, which uses credit card technology to ensure that nomadic populations stay on track with essential childhood vaccinations across borders.
The Journey Solution gives parents custodianship of their children’s electronic health data through electronic immunisation cards that health workers can swipe to see the child’s immunisation history, which is also stored in the Cloud.
“This card technology helps us run ahead of diseases. It can follow in the footsteps of the yellow cards issued for citizens of countries with a high prevalence of Yellow Fever, and can be the forerunner to a type of COVID passport for the region that will become necessary once immunisations become the norm and require tracking,” says Arunga.
The RAD project wraps up in September 2021, but was designed to enable governments, regions and their health partners to sustainably continue tracking and managing epidemic-prone diseases into the future.


 Filter resources
Filter resources